https://www.mensjournal.com/health-fitness/5-times-you-should-see-a-chiropractor-joint-pain-headaches-and-back/
CHIROPRACTIC AND MEDICARE COVERAGE: 2018-19 legislative proposal
https://www.acatoday.org/Advocacy/Legislative-Regulatory-Policy/Medicare
In the very complicated world of health insurance coverage, one little detail that is often lost to consumers is that Medicare is a beast of its own. The commercial insurance market of employer based insurance and individual policies is governed by a combination of state and federal laws. In that regard, those types of insurance are more nimble to changes in coverage. When it comes to Medicare however, this is a federally regulated benefit.
The basic Medicare chiropractic benefits were established in the 70s by Congress, and basically, they have not changed since then, in spite of the evolution of our profession to provide increased levels of complex care and long term management to our senior population. Currently only spinal adjustments for acute conditions are covered, while most commercial health plans provide a more comprehensive coverage ( albeit still with many limitations) to include evaluation/management services, supportive therapies, and extraspinal extremity care.
My standard response to patient frustrated with their Medicare benefits for the past 24 years has been to talk to your elected federal officials, since they are the only ones able to change that. Up until recently, there has been been very little interest in doing so, but the times are changing and more access to primary neuromuscular care is definitely on everybody’s mind, mostly for cost containment purposes. Our national association is making it easy for you to contact your federal reps and let them know how much you support this initiative.
Part Three: Mattress
Mattresses, even more so than pillows, are subject to personal preferences. When probed about it by patients, I often turn the question around: “If you think back about the different beds where you have slept in the past couple of years, at home and while travelling, what has felt the most comfortable to you?”. Patients sometimes need to be reminded to trust their instincts about what their body is telling them. There is a stoic mentality out there that you need a very firm mattress to support your spine. That is not entirely true. You do need a mattress with a supportive core, and one that does not fail prematurely in the center, but most people feel better with some degree of softness on the outside. The trick is to figure out how much works best for you.
There are a lot of arguments about which mattress material is best, and I don’t plan to add to that. Options range from traditional coil to layers of various materials, to structure foam of synthetic or natural origin. The durability, and often the cost of your mattress will depend upon the quality of the base material and the density of the core, especially the coils. Structure foam options are popular right now, but you need to look closely at the density per square inch on the manufacturer site, since that is highly variable and ultimately determines the firmness. Regardless of the material you chose, I recommend that you get a mattress with relatively little top layer built in and retrofit it with the top layer of your choice. This will give you the option to better customize the mattress and change the top layer halfway through the lifespan of your mattress.
From a general health standpoint, you also want to keep in mind that the newer foam materials tend to gas off a lot, especially with the fire-retardant coatings. If you are more sensitive to chemicals, you should consider the newer wool, natural rubber foam options, which unfortunately come at a steeper price point. At a minimum, you should let your new mattress gas off in a well-ventilated area for 1-2 weeks before use.
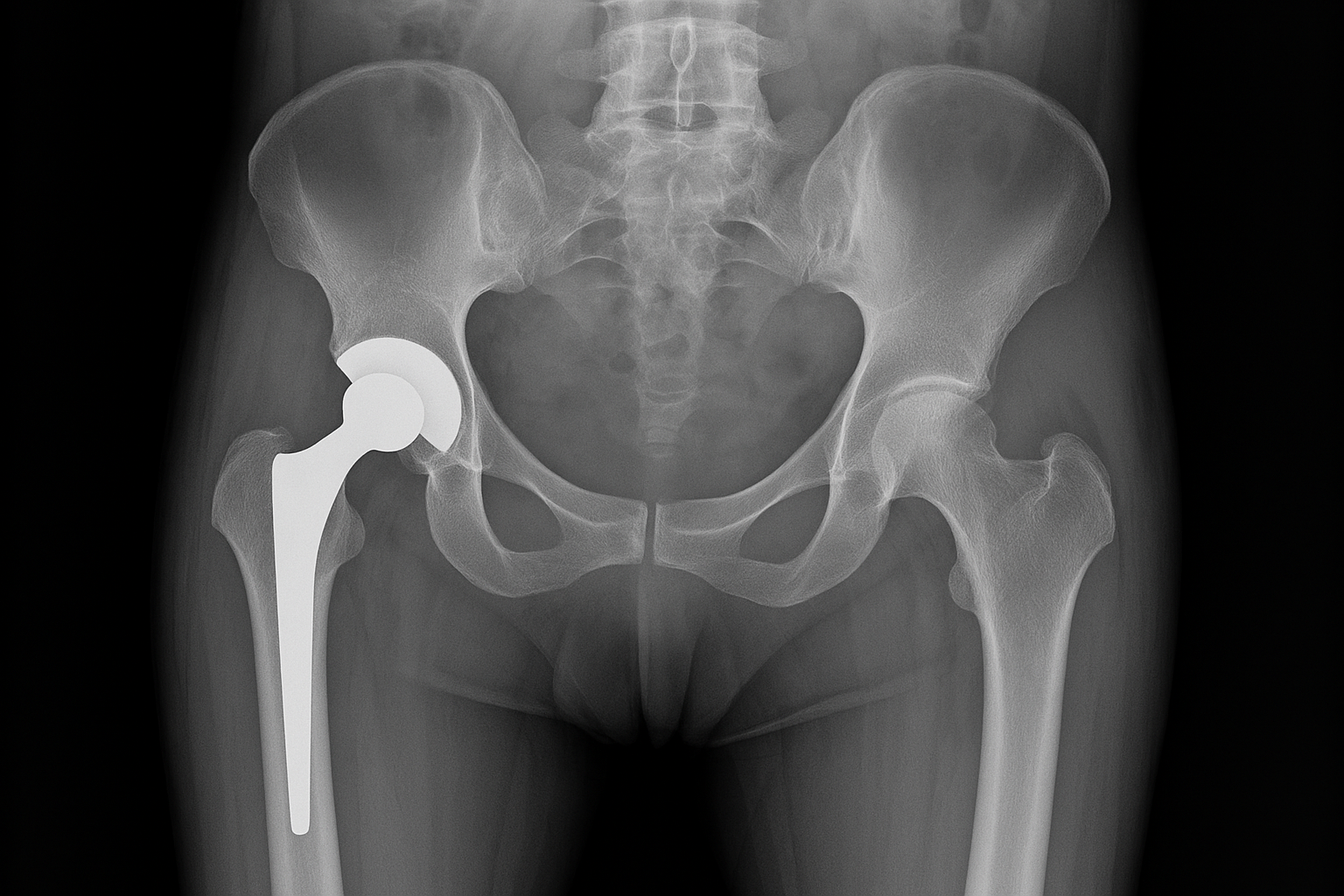
The type and thickness of the top layers becomes really crucial for patients with wide shoulders, wide hips, or any ongoing issues to the above two pressure points (shoulder impingement, prior shoulder surgery, prior hip replacement, or chronic bursitis). Less than 2 inches is usually not going to be sufficient.
The life span and support of a mattress depends a fair amount on the base of the mattress. I am not a fan of the standard box springs. They fail faster than the mattress and are mostly responsible for the middle sag of aging mattresses. The traditional European slat system is getting more readily available and cheaper. It provides an excellent combination of support and ventilation. A solid base is also an option, but it tends to limit aeration of the mattress. Flipping the mattress in both directions (180’ and upside down) every couple of months will also extend the life span of a mattress.
As a last note, bed mates sometime have widely different bedding needs and that can be a tricky problem to resolve. One easy option is a mattress with a top layer consisting of two individually controlled inflatable bladders. The other is to install two twin mattresses on a king frame and keep them connected with couple of fitted sheets or mattress protectors. Each side of the bed can be modified with the preferred mattress and top layer, and the transition between the two is usually not a significant barrier.
Part Two: Pillow Talk
I often field the question about what is the best pillow. I have to retrain the patient to ask a more important question: “What is the best pillow for me right now?”
Pillows are as individual as mattresses, there is no one-size-fits-all. Patients need to figure out what pillow will likely work for them based on their body type, existing cervical spine problems, and their sleeping position.
Sleeping position: for back sleepers, the pillow needs to be thinner to avoid pushing the head in flexion and aggravating cervical spine loss of normal curve. Ideally the pillow needs to have a slight raised edge to support the cervical curve forward and a middle dip to let the back of the head cradle back (“doughnut type pillow”). Alternately, a pillow made of a material that can be molded to shape the head/neck junction can also work (feather, foam pieces). For side sleepers, the pillow will need to be thicker to support the distance between the ear and shoulder to keep the head/neck in line with the midback. You need to subtract the distance that your shoulder will sink into your mattress, which will depend upon the weight of your trunk and the thickness of the mattress top layer.
People alternating between back and side sleeping are the most difficult to fit with the right pillow. Usually you will need a very moldable pillow or a properly sized doughnut pillow to accommodate the position change.
Body type: In order to account for the amount of compressive forces, larger trunks and heavier heads will need a heavier density pillow and conversely petite individuals can use a lighter density fill. Higher quality pillows will usually have at least two fill/density options (especially feather pillows).
Existing cervical spine issues: the firmness of a pillow is a very individual preference. By the time people show up in my office they have often tried several pillows and have already figured out what firmness works best for them. As a general rule people with active inflammatory cervical degenerative issues will need a softer, more contouring material. You can still have a firmer base such as structure foam as long as you have a couple inches of softer material on the periphery. There are a variety of softer options on the market including feather, broken foam, fillable water bladders and inflatable air bladders. The latter two options are less common but some patient enjoy the flexibility of modifying the thickness and firmness as needed.
Also remember that pillows have a relatively short life span, and usually need to be replaced every couple of years.
Sleep and Chiropractic
Sleep disruption is a pretty epidemic complaint and a topic of many questions at the office. It is a broad topic but I thought it would at least be worth highlighting some of the issues between common presenting complaint and sleep.
When patients experience pain related sleep disruption, I first have to try to understand if the problem lies with the sleep set up (bed, pillow, sleeping position), or if it is related to their intrinsic presenting neuromusculoskeletal issues. You can normally distinguish between the two by asking a few questions:
- Have you always had issues with disrupted sleep or did this recently or suddenly start? Did you have a new injury or problem before you started experiencing sleep disruption?
- Have you had any changes in bedding, mattress, pillows in the last three months? How old is your mattress?
- Do you sleep better or worse when you are not sleeping in your normal bed, such as when traveling? This question is often one that will be a big clue. If patients have the same symptoms regardless of the place where they sleep, you lean toward and intrinsic issue with their body, but if they sleep better when away from home, you start to wonder about the adequacy of their current sleep set up.
Distinguishing between a problem with the sleep set up versus the patient’s intrinsic issues and loss of tolerance to a normal bed/pillow combination is important so that you do not waste resources chasing the wrong solution.
BASIC ANTI-INFLAMMATORY PROTOCOL FOR ACUTE INJURIES
BASIC ANTI-INFLAMMATORY PROTOCOL FOR ACUTE INJURIES
As many of you know, we will often use supportive supplementation for acute injury management as well as more chronic inflammatory soft tissue management. I have gotten several requests to post the basic protocol, so here it is.
The protocol addresses three major biochemical pathways of inflammation response: vit D active metabolites, essential fatty acid cascade and the botanicals.
One important caveat: while generally safe, there are some contraindications to usage, especially in patients on any anticoagulant therapies. The dosage will also need to be adjusted a bit depending upon the acute or chronic state, and if patients are already taking some vit D as part of a calcium supplement or a multivitamin
· Vit D3 5000 IUs
· Fish oil with high EPA/DHA content: 2-3 grams/day
· High grade botanical curcumin or curcumin/ Boswellia combo. The curcumin should be at 95% concentration and the minimal dosage is 2 gr/day for 7 days in acute severe presentations ( acute disc herniation for example), 1-2 grams a day for long term presentations ( chronic inflammatory lumbar disc degeneration)
Cervical disc degeneration and smoking
I had an “interesting” conversation with a patient yesterday. We were reviewing the gentleman’s cervical X-rays and the rather surprising amount of cervical disc degeneration it showed, out of line with his age and the amount of trauma he could recall. When reviewing all risk factors for cervical degenerative disc disease, I pointed out that smoking is a big risk factors, up to 4 times the incidence versus non-smokers. Somehow that piece of information did not sit well with the gent in question, who smokes well over a pack a day and seems quite in denial about the ill effects of his habit. However, science talks louder than our denial and I forwarded him this piece of research, to let him argue with the authors if he choses. And I thought it might be a good talking point for anyone else reading this blog to have on hand
https://www.sciencedaily.com/releases/2016/02/160218062227.htm
Busting sugar
New FDA food labeling rules went into effect in July of 2018. When discussing nutrition with patients, I don't spend a lot of time on the food labeling portion since it only tells a small part of the story. Most foods that we should be eating should not present in a labeled package anyway, and other variables such as source of product, ingredient list and overall nutrient density are probably more important.
I do however welcome this new labeling rule because it finally exposes a great villain that has been living below most of our radars for too long: sugar. Some foods have inherently more sugar than others in their naturally occurring forms ( fruit for example), and while the total amount of sugar we consume matters, the quality of our sugar intake also matters. A fruit will contain a variety of other nutrients that will slow the absorption of sugar and participate in the proper conversion of sugar to energy, while plain added refined sugar does not.
The new labeling law breaks down sugar into total sugar and added sugar and the latter can be very enlightening. I recently sat down with a gentleman who was living off granola bars, assuming those were healthy meal replacement options. His favorite bar contained a whopping 15 grams of added sugar ( not even counting a total 37 gr of carbs from mostly refined grain flour). I ultimately had to convince him to switch to more whole food options such as plain nuts, fruit, boiled eggs etc... but we were also able to find some nut/fruit bars that had less than 5 grams of added sugar and were still palatable to him when grabbing something on the go.
The current recommendation is for less than 50 grams of added sugar per day. I would say that optimally that is even high and we should aim closer to 30-40 grams. But considering that most US adult get around 150 on average right now, I would be satisfied with just 50 grams
https://www.npr.org/sections/thesalt/2016/05/20/478837157/the-added-sugar-label-is-coming-to-a-packaged-food-near-you